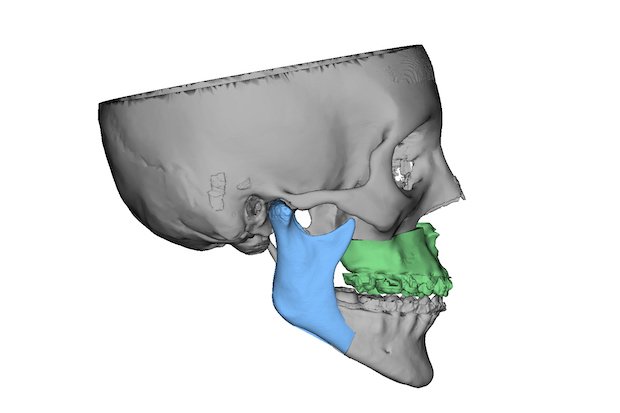
3D Systems software showing the final positions in a virtual surgery.
It is estimated that 20% of the populations suffer from some level of craniofacial defect. In the majority of these cases orthodontal care (braces, aligners etc.) is sufficient but roughly 5% of those require corrective jaw surgery or orthognathic surgery.
Despite its commonality the process of removing bones, reshaping them and moving them does, as you’d imagine, have its complexities. Recent advancements in technology, and in particular 3D technology, have greatly increased accuracy and reducing operating times.
In one particular case, performed by Deepak Krishnan, DDS, of Cincinnati’s UC Health, the patient presented with a unilateral cleft lip and palate. The patient was diagnosed with maxillary hypoplasia, mandibular hyperplasia, and facial asymmetry resulting in the inability to chew properly, poor speech, and disfigurement.
Double-jaw surgery was scheduled and pre-planned using 3D Systems’ VSP (Virtual Surgical Planning) Orthognathics service.
The digital 3D models that serve as the foundation of VSP provide clinicians with a more complete view of the intrinsically unique anatomy of each patient. This enables the presiding surgeon to accurately visualise and analyse patient-specific anatomical discrepancies, explore multiple treatment options for each patient, and visualise, anticipate and prepare for possible surgical obstacles prior to beginning the surgery
Planning a surgery with VSP Orthognathics begins by sending medical imaging data of the patient, produced using CT or CBCT technology, to 3D Systems to create a digital 3D model of the patient’s precise anatomy. For this surgery, dental models were also overlaid on a CT scan to ensure the best possible occlusion was achieved.
The patient-specific 3D rendered anatomy is then shared online with 3D Systems biomedical engineers. Using 3D software to manipulate the digital model of the patient’s anatomy in real-time, the group can analyse patient discrepancies, simulate surgical osteotomies, perform bony movements and assess potential surgical complications. The placement of reconstructive plates or bone grafts can also be accurately simulated within VSP online sessions in cases where they are prescribed.
Dr Krishnan pre-planned the surgery with assistance from 3D Systems’ VSP Orthognathics team by talking through the sequence of movements he wanted to make to deliver the patient’s ideal anatomical correction. “VSP planning sessions are invaluable to understanding the patient anatomy and details,” says Dr Krishnan. “The ability to consider different treatment alternatives during the planning is also immensely helpful. I was able to explore several options for this patient with the VSP engineer before choosing the one I felt was best to implement.”
As Dr Krishnan requested each movement, the 3D Systems’ engineer updated the digital model in real-time to reflect the desired outcome. At the end of Dr Krishnan’s web session, each surgical update and obstacle had been accounted for to enable the outcome D. Krishnan planned to deliver.
Transferring the pre-surgical plan to the operating room
After the online planning session, 3D Systems’ biomedical engineers designed and SLA 3D printed the occlusal splints Dr Krishnan would use in surgery to correctly place the bony anatomy. The SLA splints are sterilised by the surgical teams prior to use in the operating room.
In the VSP planning session Dr Krishnan decided to move the mandible first, so an intermediate splint was created to relate the upper teeth to the lower teeth. Once the mandible was positioned in surgery according to the digitally pre-planned movements, the surgical team fixated it there using plates and screws.
Following the intermediate splint, a second and final splint was used to bring the upper jaw to meet the lower jaw, putting the patient into the correct occlusion.
Dr. Krishnan says VSP enabled him to save time in the operating room by determining his exact movements ahead of time. “The patient-specific splints ensured that the planned moves were executed and minimised the intra-operative carpentry.”
